Researchers investigate the causes of polycystic ovary syndrome
Pregnancy and child
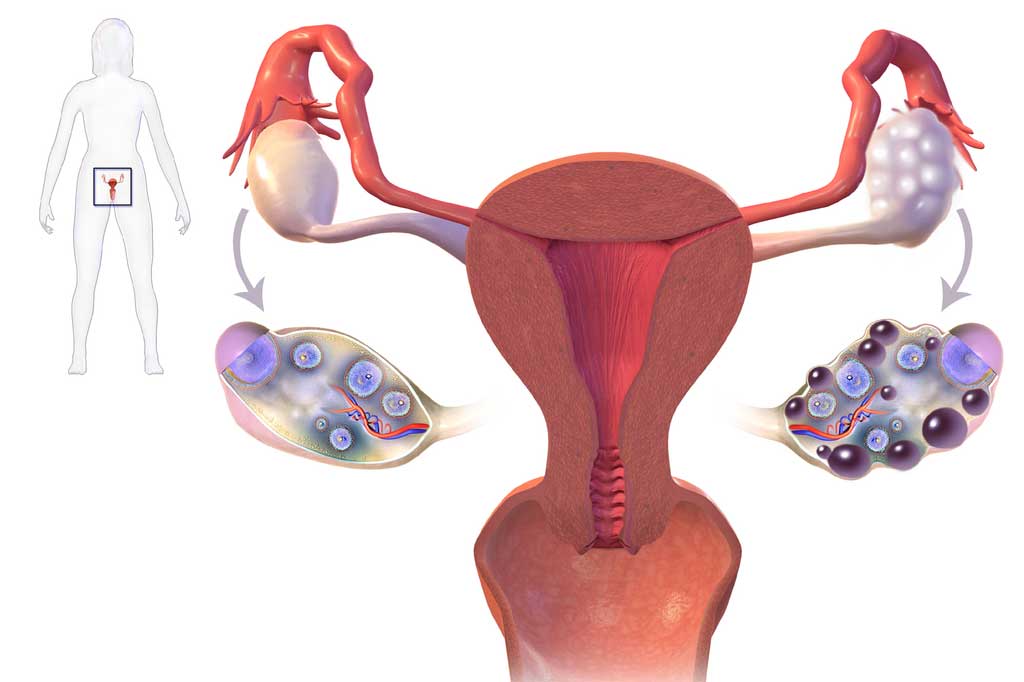
'A common cause of female infertility - polycystic ovary syndrome (PCOS) - may be due to a hormonal imbalance before birth, researchers have found' BBC News reports
"Fertility hope for polycystic ovary sufferers," the Mail Online reports.
This is a simplistic interpretation of a complex study that aimed to investigate hormone imbalances in pregnant women with polycystic ovary syndrome (PCOS), and the possibility these women could pass PCOS on to their daughters.
PCOS is thought to be related to abnormal hormone levels and can cause irregular (or sometimes no) periods, weight gain and difficulties getting pregnant.
Researchers specifically looked at a hormone called anti-Mullerian hormone (AMH). AMH is produced by the ovaries when they release an egg as part of the menstrual cycle.
AMH levels are normally low during pregnancy as the ovaries aren't releasing eggs. But this study found pregnant women with PCOS had high levels of AMH.
The researchers wanted to see if these high levels of AMH could cause the condition in daughters, possibly by disrupting their development when they were still in their mothers' womb.
The researchers injected AMH into pregnant mice, and their offspring had symptoms of polycystic ovaries.
These offspring were given cetrorelix, a drug used in IVF treatment to prevent ovulation until the optimal time for conception.
Cetrorelix works by blocking another hormone, gonadotrophin. Gonadotrophin levels are known to be raised in women with PCOS.
Giving the drug did reduce symptoms of the condition in the offspring mice.
But the results of this research are hard to interpret and do not yet provide "fertility hope" for women with PCOS.
Giving cetrorelix would simply prevent ovulation and is not a treatment for the fertility problems associated with PCOS.
Where did the story come from?
The study was carried out by researchers from medical laboratories and universities in France, Sweden, Finland and Italy.
It was funded by the European Research Council under the European Union's Horizon 2020 research and innovation programme, the French National Institute of Health and Medical Research, the French National Agency of Research, the Lille Regional University Hospital in France, and a European Research Fellowship.
It was published in the peer-reviewed journal Nature Research.
The UK media reported on the findings of this study fairly accurately.
Both the Mail Online and BBC News make it clear that this research was mostly carried out using mice, although the Mail Online stating that this study offers "fertility hope" is a little misleading.
What kind of research was this?
This was a laboratory study where the researchers primarily wanted to see if PCOS is passed on from one generation to the next.
They first tested blood samples from a cohort of pregnant women with and without PCOS.
They then carried out further tests to investigate their theories first in pregnant mice, then in the offspring from that pregnancy.
While research in mice can provide preliminary data and important clues that may give an idea of biological processes, it does not automatically translate to what will happen in the human body.
What did the research involve?
The researchers took a sample of 63 healthy pregnant women and 66 pregnant women with PCOS. All the women were 16 to 19 weeks pregnant.
They measured levels of anti-Mullerian hormone (AMH) in both groups. These levels are normally low in pregnancy because the ovaries aren't being stimulated to release eggs.
Then the researchers conducted an experiment in mice. They injected AMH into pregnant mice to create the same hormone imbalances found in PCOS.
As the resultant baby mice grew up, the researchers checked for signs of PCOS.
If the baby mice had PCOS, they treated them with cetrorelix, a drug used in IVF to control women's hormones.
This drug blocks the action of gonadotrophin hormones that stimulate the ovaries to release eggs before they can be collected for IVF.
In women with PCOS, levels of gonadotrophin hormones are often raised. The researchers therefore wanted to see if blocking these hormones had any effect on symptoms of PCOS.
What were the basic results?
The researchers showed that levels of AMH were higher in women with PCOS than in healthy women.
In the mice study, the babies of the pregnant mice injected with AMH showed symptoms of PCOS as they grew up – for example, they had higher testosterone levels.
Following treatment with the IVF drug cetrorelix, the baby mice stopped showing these symptoms.
How did the researchers interpret the results?
The researchers stated that these findings highlight the role of excess foetal exposure to anti-Mullerian hormone during pregnancy.
They also suggested the possibility of giving gonadotrophin-blocking treatment to treat and prevent PCOS.
Conclusion
PCOS is by far the most common hormonal condition affecting women of reproductive age, and a common cause of fertility problems.
But it's too early to say that drugs like cetrorelix could be a potential treatment.
The drug has only been tested in mice. The way diseases develop and respond to treatment is not identical in mice and humans.
While we know that levels of gonadotrophin hormones are raised in women with PCOS, blocking these hormones is not an established treatment for the condition.
The fact that blocking gonadotrophin decreased some PCOS symptoms in mice doesn't automatically mean it would cure the condition in women.
When it comes to fertility, the drug would prevent ovulation altogether, so it's unclear what role it could have.
These findings are of interest, but much more research is needed to see whether cetrorelix could be put into early clinical trials in humans.
Anyone concerned about symptoms of PCOS or with a family history of PCOS should see their GP.
Find out more about PCOS






 Subscribe
Subscribe Ask the doctor
Ask the doctor Rate this article
Rate this article Find products
Find products






